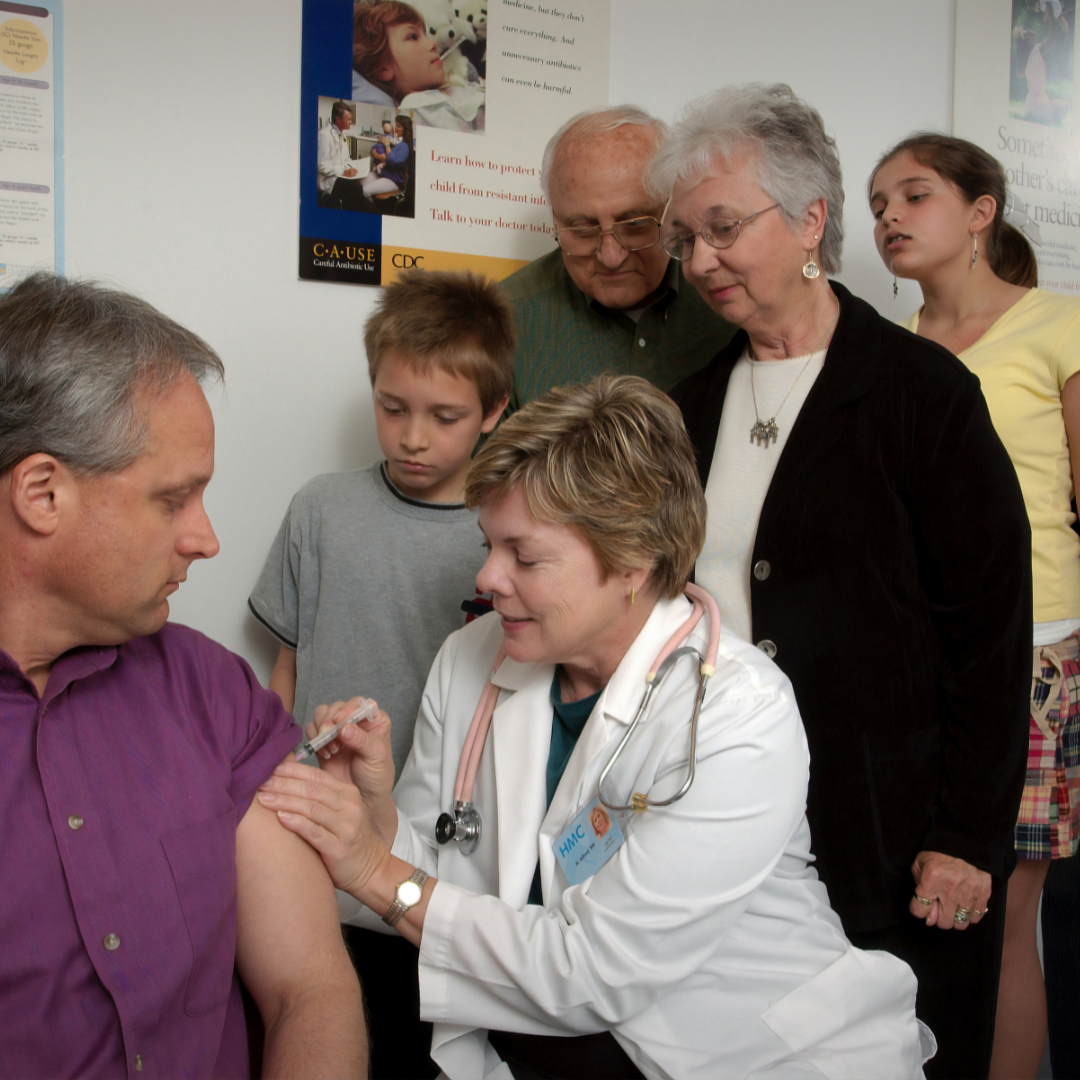
Any health plan that meets the requirements of the Affordable Care Act (ACA) is considered minimum essential coverage. The Children's Health Insurance Program (CHIP) and Medicare and job-based health insurance are all eligible insurance plans.
Earlier, you had to pay a tax penalty if you didn't obtain minimum essential coverage or qualify for an exemption under the original law. Despite federally eliminating the penalty in 2020, some states still impose fees on those without minimum health coverage.

Let’s take a look at the quick links in this article:
- What is a minimum essential coverage?
- What are the 10 minimum essential benefits?
- Do you need minimum essential coverage?
- What are the MEC requirements?
- What is not considered minimum essential coverage?
- HRAs and minimum essential coverage
- Significant Modifications to Minimum Essential Coverage
- FAQs
- How can Deskera Help You?
- Key Takeaways
What is a Minimum Essential Coverage?
Under the Affordable Care Act, any health plan that qualifies and meets the ACA's requirements is termed minimum essential coverage. According to the Affordable Care Act (ACA), a qualified health plan must follow federal regulations regarding deductibles and copayments. It must be certified by the federal health insurance marketplace and cover ten essential health benefits.
What are the 10 minimum essential health benefits?
According to the ACA, health insurance plans must cover ten essential health benefits. Let's take a look at the list comprising the 10 essential health benefits here:
- Outpatient care
- Emergency services
- Hospitalization
- Pregnancy, maternity care, and newborn care
- Mental health care services and services for substance use ailments
- Prescription drugs
- Rehabilitation services and devices
- Laboratory services
- Preventive, wellness, and chronic disease services
- Pediatric services
Who needs minimum essential coverage?
When you live in the United States or abroad, qualify for tax reasons as a resident alien needs minimum essential coverage. Additionally, if you are a permanent resident or both, you need minimum essential coverage. However, it does not include the individuals residing in the U.S. territories; they are exempt from this requirement.
What are the Minimum Essential Coverage requirements?
We have already learned that the federal law no longer imposes penalties for not having health insurance. Despite this fact, it is necessary to maintain active health insurance coverage.
One may ask how to meet the ACA minimum essential coverage requirement. It is essential to enroll in a health plan that meets minimum essential coverage requirements. Plans available through the marketplace, Medicare, job-based coverage, Medicaid, and CHIP can all be examples here.
The following sub-section comprises a list of plan types that meet the ACA coverage requirements.
For Individual, family, or employer plans
- Health insurance plans obtained through a state or federal exchange
- The purchase of individual health insurance plans outside an insurance exchange that meet the requirements for qualified health plans
- Grandfathered plan purchased outside a health insurance exchange
- COBRA and retiree health plans sponsored by employers
- Protection under the health insurance plan of a parent
- Student health insurance plans
State or Federal Insurance Plans
- Medicare Part A
- Medicaid coverage, except those with limited coverage
- Medical coverage for Peace Corps volunteers
- Medicare Advantage plans, or the Medicare Part C
- Specific plans which are offered by the Department of Veterans Affairs (VA)
- Most TRICARE plans, also called uniformed services health care programs
- Health Benefits Program for Defense Non-appropriated Funds (DoD NAF)
- Children's Health Insurance Program (CHIP)
- Health insurance for refugees through the Administration for Children and Families
What is not considered minimum essential coverage?
So far in the article, we have been reading about the minimum essential coverage requirements in depth. Now, we will learn about the plans that are not considered under the minimum essential coverage category.
Here are the reasons why certain plans are not placed under the minimum essential coverage category:
- The plans that do not offer any essential health benefits are not placed under the minimum essential coverage category
- They do not cover preexisting conditions
- These plans are not regulated by the ACA
- They offer only vision and dental coverage
- They offer only Workers' compensation
- Offer coverage only for a specific disease or condition
- These are plans that provide only discounts on medical services are also not placed under the minimum essential coverage category
HRAs and Minimum Essential Coverage
HRAs or Health Reimbursement Arrangements are an alternative for companies that are unable to offer group health coverage to their employees.
HRAs reimburse employees for some or all of their qualified health expenses up to a fixed annual amount. HRAs offer the advantage of enabling you to roll over unused HRA funds for future use in some HRAs. The employees submit receipts to the HRA for reimbursement based on the services received. Furthermore, the reimbursements made to employees are not taxable.
Small Business Advantage
A QSEHRA or Qualified Small Employer HRA is specially designed for small businesses. As prescribed by the IRS, it is intended for businesses with fewer than 50 full-time employees. Businesses that want to provide QSEHRA to their employees must ensure that they:
- Do not offer any group health insurance or
- Also, they do not provide a health flexible spending account (FSA)
Apart from this, another crucial aspect related to QSEHRA is the eligibility of the employee. The employees must have health insurance that meets minimum essential coverage as defined by the ACA. This fulfills eligibility criteria for the employees to enroll for QSEHRA.
Significant Modifications to Minimum Essential Coverage
The Tax Cuts and Jobs Act (TCJA) has implemented significant changes to minimum essential coverage. Let’s take a look at those points here:
- It eliminated the penalty for not having MEC. 2018 was the last year for which individuals would be subject to the penalty. From 2019 forward, the minimum essential coverage mandate remained in effect.
- Uninsured individuals, however, are no longer subject to penalties. QSEHRA participants must still have MEC plans even though there is no longer an individual mandate.
- A number of states have challenged the Affordable Care Act as a whole since the TCJA nearly eliminated the penalty.
- In November 2020, the Supreme Court will hear a case challenging the constitutionality of the Affordable Care Act, California v. Texas.
- Because of the repeal of the individual mandate, the Supreme Court may reverse its decision in NFIB v. Sebelius, under which the ACA could tax. This could greatly impact both employers’ and individuals' current health insurance requirements.
FAQs
This section comprises frequently and commonly asked questions regarding the minimum Essential coverage. Let’s look at them:
Q: Is proof of minimum essential coverage required for my tax return?
With federal taxes filed in and after 2020, you are not required to provide proof of minimum essential coverage. Furthermore, the federal health coverage exemption will also be discontinued in 2020 as federal penalties will no longer apply.
Q: Will I be covered by minimum essential coverage if I am covered by my spouse's employer?
Yes. Employer-sponsored insurance generally meets the minimum essential coverage requirements. When an employee enrolls in employer-sponsored health insurance for himself and his family, all covered family members are covered to the minimum essential standard.
Q: Do you know what the minimum essential coverage for non-ESI is?
An organization other than the employer provides health insurance is known as non-ESI minimum essential coverage. Examples of this are Medicaid and Medicare. Occasionally, HealthCare.gov will use this term to inform you that you are conditionally eligible because you are enrolled in non-ESI coverage. Upon receiving such a notice, you will have 90 days to deliver documents explaining your condition.
Q: I was told that my employer's health plan is grandfathered. Is this minimum essential coverage?
A: Yes. Group health plans with grandfathered coverage are minimum essential coverage.
Q: My age makes me ineligible for Medicare as a retiree. I am covered by a retiree health plan provided by my former employer. Does it provide minimum essential coverage?
A: Yes. Most retiree health plans provide minimum essential coverage.
How can Deskera Help You?
Deskera People allows you to conveniently manage leave, attendance, payroll, and other expenses. Generating pay slips for your employees is now easy as the platform also digitizes and automates HR processes.
Key Takeaways
- Any health plan that meets the requirements of the Affordable Care Act (ACA) is considered a minimum essential coverage
- Under the Affordable Care Act, any particular health plan that qualifies and meets the ACA's requirements is termed minimum essential coverage. According to the Affordable Care Act (ACA), a qualified health plan must follow federal regulations regarding deductibles and copayments
- Emergency services, Hospitalization, Pregnancy, maternity care, and newborn care, Mental health care services, and services for substance use ailments are among the 10 minimum essential health benefits
- When you live in the United States or abroad, qualify for tax reasons as a resident alien will need to have minimum essential coverage
- Additionally, if you are a permanent resident or both, then you need minimum essential coverage
- The plans that are not regulated by the ACA are not considered under minimum essential coverage
- HRAs or Health Reimbursement Arrangements are an alternative for companies that are unable to offer group health coverage to their employees
- A QSEHRA or Qualified Small Employer HRA is specially designed for small businesses. As prescribed by the IRS, it is intended for businesses with fewer than 50 full-time employees
- The Tax Cuts and Jobs Act (TCJA) made significant changes to minimum essential coverage, which includes eliminating the penalty for not having MEC
Related Articles